In healthcare, following rote procedures doesn't always cut it. To treat the whole human, you have to account for subjective realities. It's no secret that the way patients experience, perceive, and respond to treatment makes a huge difference in outcomes.
Topics: Urodynamics Testing, urodynamics staffing
The Role and Significance of Urodynamics Testing in Urology
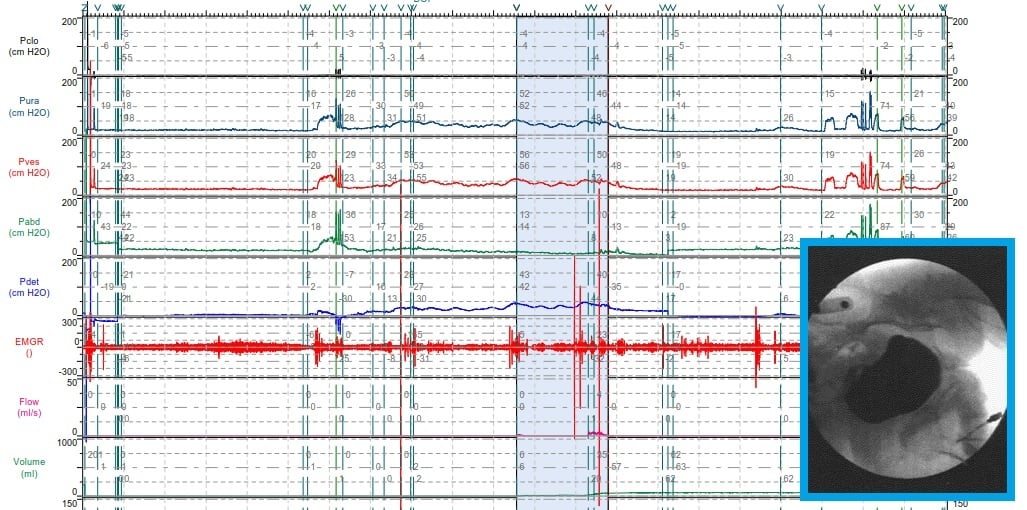
Urodynamics testing exposes the key relationships between the lower urinary tract and how well people retain and pass urine. These diagnostic procedures reveal the underlying connections you can't see just by looking — the changing conditions and health factors hidden inside the sphincter, bladder, and pelvic floor muscles.
Topics: Urodynamics Testing
 The lower urinary tract does quite a lot. Urodynamics testing gives your urologist, urogynecologist, or physician the insights needed to understand how your urinary system functions — and whether you might need treatment.
The lower urinary tract does quite a lot. Urodynamics testing gives your urologist, urogynecologist, or physician the insights needed to understand how your urinary system functions — and whether you might need treatment.
Topics: Urodynamics Testing
Transforming Houston Healthcare: Urodynamics and Specialty Diagnostics
The landscape of healthcare, particularly urodynamics, in the rapidly evolving city of Houston presents a fascinating dichotomy. As a diverse global hub, Houston's unique population brings complex and varying health needs, making the delivery of Houston healthcare a formidable challenge. The urological health concerns presented by Houston area patients can range from those influenced by cultural and behavioral factors, to those exacerbated by economic circumstances, culminating in a rich, multifaceted tableau of patient profiles. Our approach to providing urodynamics in the Houston area factors in and compensates for this complexity.
Topics: Urodynamics Testing, Urodynamics Nurse
Pelvic Floor Physical Therapy - Why Is It Not More Widely Adopted?
Pelvic floor muscles work with the pelvic bones to support your lower body. Like the muscles that help you lift, they stabilize your pelvis and spine while improving pelvic floor strength. They are extremely important, especially in women during pregnancy, delivery, and recovery. They can also help you with incontinence, sexual function, and even your ability to walk.
However, due to trauma and stress, the pelvic floor muscles can become weakened or tight, leading to pelvic floor disorders, such as stress urinary incontinence and pelvic organ prolapse. These disorders are widely known and can significantly impact women's health and quality of life.
5 Ways Urologists Can Grow Their Primary Care Referral Networks
Practitioners have no shortage of public outreach options – but some strategies drive business more effectively than others. Whether you're trying to augment your patient base or build relationships with other healthcare providers in the community, expanding your primary care referral network is a good start.
Establishing a strong referral network can empower your brand to go further and reduce your marketing burden, freeing you to focus on caregiving. Here are five ways to drive referrals and help your practice succeed.
How Urodynamics Furthers Understanding of Stress Urinary Incontinence
Urinary incontinence is the involuntary leakage of urine. Although it's commonly associated with geriatric health issues, this isn't just something that affects the elderly. For instance, it's more common among women than men – yet regularly used women's treatment plans often prove suboptimal.
There are a few major types of urinary incontinence, including urge, stress, and mixed. With stress urinary incontinence (SUI), caregivers and patients have access to a wide range of treatment options, but it's vital to get the diagnosis right first – and urological medicine plays a major role in effective treatment.
Topics: Urodynamics Testing, stress incontinence
Most medical practitioners are well aware that few procedures are truly risk-free. While this seems obvious in the case of things like surgeries, treatment isn't the only area of concern when it comes to patient outcomes. Certain diagnostic procedures may also pose risks, making it vital to understand how to mitigate the hazards and optimize the quality of treatment.
Urodynamic studies (UDS) are a prime example of how an overwhelmingly benign procedure nonetheless demands attention to detail and experienced oversight. Here's what to know about UDS, conditions like bacteriuria and urinary tract infections (UTIs), and commonplace risk reduction strategies like the use of prophylactic antibiotics.
Topics: Urodynamics Testing
Urodynamics is a set of tests and procedures that measure lower urinary tract function. These tests are prescribed by urologists, gynecologists, or urogynecologists, and the results from the tests allow them to look at how a patient's lower urinary tract is working. The bladder, sphincters, and urethra (all parts of the lower urinary tract) work together to hold and release urine. Most urodynamic tests are concerned with measuring the ability of your bladder to hold and drain urine completely.
Topics: Urodynamics Testing, urodynamics equipment, urodynamics training
Urodynamics is a panel of tests relating to the lower urinary tract. It is most commonly used in its entirety; however, it is also possible that one or more of the components will be performed separately if symptoms suggest this is necessary.
Urodynamics is the most reliable way to determine the cause of lower urinary tract symptoms and therefore, the best way to determine which treatment methods are most appropriate.
A Care Pathway is an evidenced-based framework to build a treatment plan upon, beginning with the primary physician, continuing to specialist referrals if necessary, and following the patient through to the end of their treatment (including follow-up care).
They typically follow a common path that starts with patient history, followed by clinical assessment, provisional diagnosis, first line management, specialist management, and follow-up care.
Some examples are listed here:
Topics: Urodynamics Testing, General Urology Information, urodynamics, urodynamics equipment, urodynamics staffing, urinariy incontinence, urodynamics interpretation, post-void residual, stress incontinence, urodynamics profitability, urodynamics catheters, UroGynecology, Cystometrogram