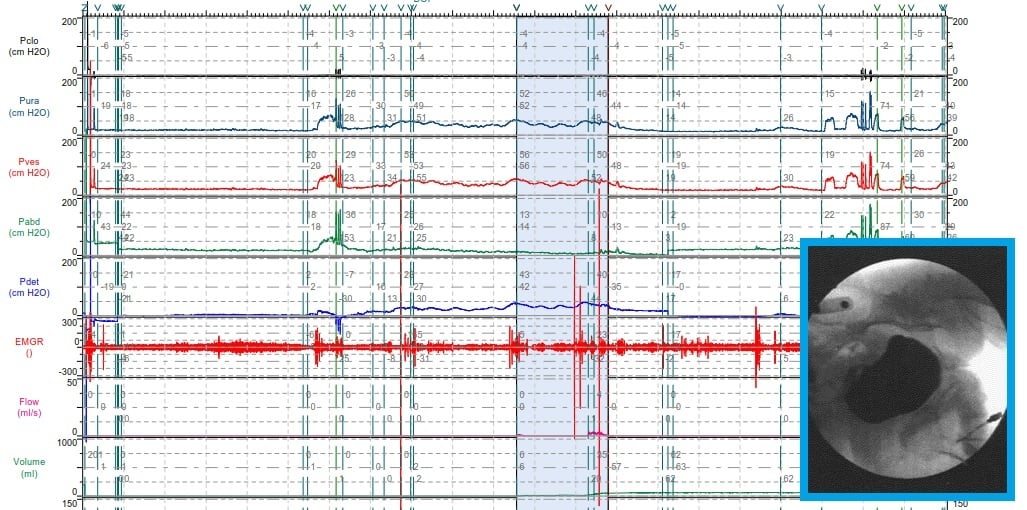
Urodynamics testing is the process of evaluating a range of bladder, urethra, and pelvic floor diagnostics. Accurate diagnosis of related health conditions requires careful examination of each component's very specific functions, and urodynamics testing includes numerous specific strategies for doing so.
Clark Love
Recent Posts
A Full 2024 Explanation of Urodynamics Related CPT Codes
Topics: urodynamics billing
Numerous issues can arise in the lower urinary tract, and the underlying pathologies of these diseases and conditions can be complex and unclear. Urodynamics is crucial in enhancing diagnostic accuracy and patient outcomes.
Like other diagnostic tools, urodynamics requires thorough training. Substantial data is produced, and its accuracy relies heavily on precise administration techniques.
Training is vital for healthcare professionals aiming to utilize urodynamics to assist patients. However, developing and implementing a comprehensive curriculum is a challenging task.
Where can your practice seek guidance? Many practitioners rely on established providers like Laborie and Brighter Health Network. If you are new to urodynamics training, here is what to consider when looking for an effective program.
Topics: urodynamics training
Navigating Regulatory Compliance in Urodynamics Testing
Practice administrators and physicians can't take compliance for granted. The more the medical profession evolves, the more the legal landscape seems to shift in kind. But treatment is far from the only area where this matters. The diagnostic side also demands close regulatory management.
What makes a good governance and regulatory compliance strategy? The ideal looks different for each practice, but it's wise to understand a few highlights.
Topics: Urodynamics compliance
In healthcare, following rote procedures doesn't always cut it. To treat the whole human, you have to account for subjective realities. It's no secret that the way patients experience, perceive, and respond to treatment makes a huge difference in outcomes.
Topics: Urodynamics Testing, urodynamics staffing
The Role and Significance of Urodynamics Testing in Urology
Urodynamics testing exposes the key relationships between the lower urinary tract and how well people retain and pass urine. These diagnostic procedures reveal the underlying connections you can't see just by looking — the changing conditions and health factors hidden inside the sphincter, bladder, and pelvic floor muscles.
Topics: Urodynamics Testing
Urology and ChatGPT - Probing ChatGPT's Understanding of Urodynamics
If you've been reading the news, you've noticed we're in sort of an AI craze, and ChatGPT is undoubtedly one of the star players. This large language model (LLM) has been praised and reviled for its seeming ability to compose text, answer questions, and solve problems. Considering that people are building apps to answer complex legal, financial, scientific, and even medical questions with the bot, it stands to reason to ask: What will the healthcare ramifications be?
 The lower urinary tract does quite a lot. Urodynamics testing gives your urologist, urogynecologist, or physician the insights needed to understand how your urinary system functions — and whether you might need treatment.
The lower urinary tract does quite a lot. Urodynamics testing gives your urologist, urogynecologist, or physician the insights needed to understand how your urinary system functions — and whether you might need treatment.
Topics: Urodynamics Testing
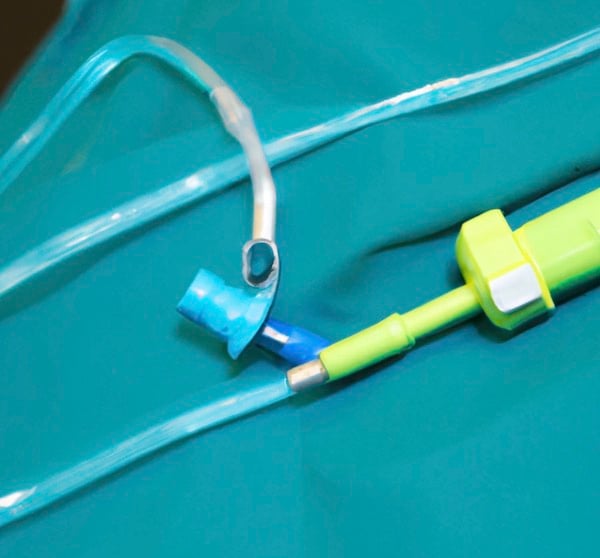
Conflict comes in many forms, and urology practices aren't immune to the fallout. From friendly rivalries to all-out supplier wars, this field packs more competitive punch than you might expect. The ongoing battle over urodynamics catheters from Laborie Medical and Gemini Medical couldn't be a better example.
What do urodynamics catheters — something you'd assume might be relatively uncontroversial — have to do with what's shaping up to become a massive market brouhaha? And could urology practices benefit no matter who comes out on top? Let's dive into the battle to find out more — from a safe distance, of course.
Topics: urodynamic catheters
Urodynamics testing expands the range of diagnostic data available to urologists. By making it easier to associate numbers with observations, urodynamics enhances the speed, accuracy, and repeatability of common diagnostic procedures.
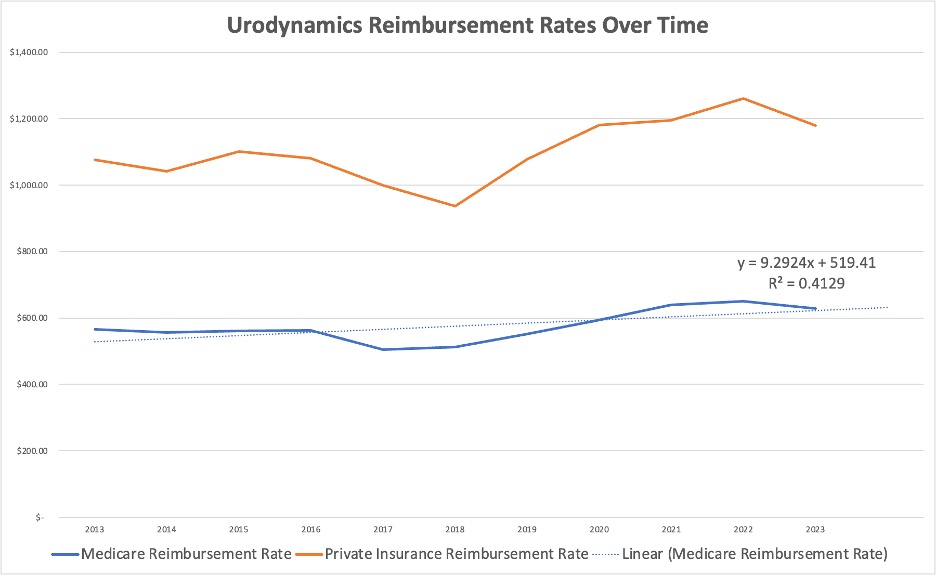
Urodynamics Reimbursement Rates: 10-year Trend and Future Projections
Want to understand what's coming down the line for professionals who specialize in urodynamics? Don't just look to new diagnostic technologies or evolving caregiving practice standards. Urodynamics reimbursement rates are also a great bellwether of practice viability.
Topics: Reimbursement Trends, Urodynamics Reimbursement Rates