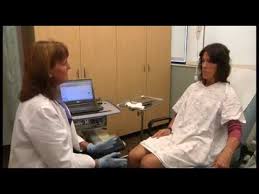
Numerous issues can arise in the lower urinary tract, and the underlying pathologies of these diseases and conditions can be complex and unclear. Urodynamics is crucial in enhancing diagnostic accuracy and patient outcomes.
Like other diagnostic tools, urodynamics requires thorough training. Substantial data is produced, and its accuracy relies heavily on precise administration techniques.
Training is vital for healthcare professionals aiming to utilize urodynamics to assist patients. However, developing and implementing a comprehensive curriculum is a challenging task.
Where can your practice seek guidance? Many practitioners rely on established providers like Laborie and Brighter Health Network. If you are new to urodynamics training, here is what to consider when looking for an effective program.