Urodynamics Explained
Urodynamics is a blanket term for a series of tests that assess the functionality of the lower urinary tract. Numerous
problems of the bladder and urethra which commonly affect both men and women can be diagnosed via urodynamics. Typically, these tests are ordered to diagnose issues such as urinary incontinence or prostrate problems, as well as before and after any type of surgery involving the pelvic organs or the urinary tract. Common symptoms that result in a doctor ordering urodynamics include incontinence, frequent urination, inability to urinate, weak urine stream, painful urination, nocturia, recurrent urinary tract infections, and difficulties emptying the bladder entirely. The types of urodynamic tests commonly performed include the following:
- Uroflowmetry is a test which measures a patient’s natural urine flow rate, as well as urine volume before and after voiding. Here, the patient is asked to empty his or her bladder naturally while a flow rate meter records urine flow. This test is routinely performed for all urodynamic assessments, and is useful when diagnosing the cause of weak urine stream or difficulty urinating. Additionally, uroflowmetry can determine how well a patient’s bladder and sphincter are functioning, and can be used to determine if obstructions are blocking the bladder from releasing urine.
- Pressure uroflowmetry is like uroflowmetry described above in that it also measures the rate of urination. However, bladder and rectal pressures are also simultaneously recorded during this assessment. Pressure uroflowmetry requires invasive catheterization and is useful for diagnosing disorders that result in difficulty urinating. Common diseases that are diagnosed with this test are bladder muscle weakness and bladder outlet obstruction.
- Post-void residual volume tests are used to measure the volume of urine that remains in the bladder after voiding. This test is important in the assessment of many urinary tract disorders. Here, the patient is asked to void his or her bladder naturally, and then a bladder scanner is used to noninvasively measure the amount of urine remaining in the bladder. If a bladder scanner is unavailable, the patient is catheterized and the remaining amount of urine is measured. Post-void residual volume assessments are primarily used to determine neurogenic bladder disorders as well as the cause of frequent urinary tract infections, renal insufficiency, bladder outlet obstruction, and detrusor underactivity.
- Multichannel cystometry is a type of pressure uroflowmetry test. Two pressure catheters are inserted, one in the bladder and one in the rectum, to measure associated pressures during both the filling and emptying of the bladder. Assessments that are made include the presence of contractions in the bladder wall during filling or stress (i.e. coughing), urethra strength, detrusor under- or overactivity, and bladder outlet obstruction. This test is the gold standard for diagnosing stress urinary incontinence.
- Electromyography is a test that measures the electrical activity in the bladder neck. It can be performed during voiding to determine coordinated or uncoordinated voiding and the functioning of the detrusor muscle. For this measurement, electrodes are placed in the pubic area of the patient to test for electrical impulses from the muscles. Most commonly, electromyography is beneficial when testing for neurologic disorders that affect the communication between the brain and body.
- Urethral pressure profilometry measures strength of sphincter contractions. This test is used to further study urinary incontinence in both men and women.
- Fluoroscopy (also known as videourodynamics) is a moving video x-ray of the bladder and bladder neck that is obtained while the patient is voiding her bladder. This test helps doctors provide a better view of what is happening in the lower urinary tract, such as bladder outlet obstruction or pelvic organ prolapse.
Ultimately, each of the tests described above is important for diagnosing various disorders of the lower urinary tract. These tests range from non- to minimally invasive and are performed as outpatient procedures. There is minimal pain or discomfort associated with each assessment, and few risks involved, which will be explained in more detail below. Additionally, doctors are typically able to provide patients with immediate answers regarding their urinary symptoms.
Drawbacks of Urodynamics
Although urodynamic testing is performed frequently and with confidence, there are a number of drawbacks associated with this assessment of the lower urinary tract in this manner. Limitations include: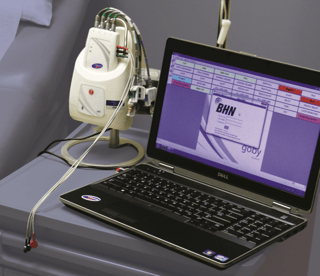
Risk of Infection
Urodynamics requiring catheterization is an invasive procedure. The main side effect experienced by patients is urinary tract infection, caused by introduction of bacteria via the catheter, or potential for superficial damage (i.e. cuts or scrapes) during insertion. Other possible side effects include damage to the urethra or bladder.
Discomfort
Patients are often reticent to undergo urodynamic testing due to the risk of discomfort and embarrassment. Indeed, male patients cite pain as one of the top reasons to avoid catheterization. Since testing requires patients to have their genitals handled by nurses and physicians, many also find urodynamic testing mentally or emotionally uncomfortable.
Technical Difficulties
Urodynamics involves many moving parts, and artifacts in measurement can easily occur. Air bubbles, patient movement, and poor catheter or electrode placement can all cause artifacts in the measurements and poor data. This problem is so pronounced that entire seminars are devoted to proper urodynamics technique, yet even the best urodynamic technicians still encounter problems occasionally.
Cost
Urodynamics can be a costly procedure, as it requires specially trained staff as well as use of special equipment.
InterpretationAdditionally, urodynamic results are sometimes subjective due their openness to interpretation. Two doctors may interpret the same result differently, which can lead to misdiagnoses.
UroCuff: A Noninvasive Solution
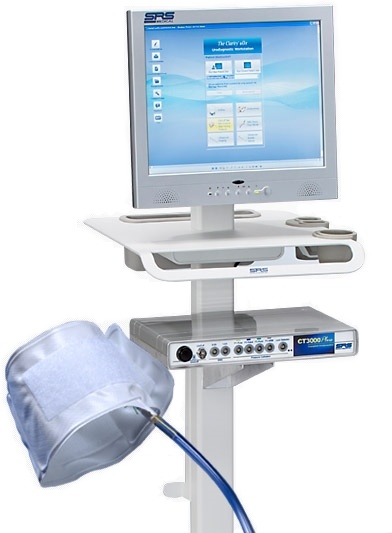
The UroCuff is a piece of urodynamic equipment that can be utilized to non-invasively measure urine flow rate and bladder pressure, as well as aid in the diagnosis of voiding disorders. A small, pneumatic cuff is fitted around a patient’s penis before the bladder is voided. Then, the patient urinates into a portable toilet that is fitted with a flow meter. While the patient is urinating, the cuff is automatically inflated until the patient’s urine stream is interrupted. The inflation and interruption cycle is repeated until voiding is complete. The pressure applied to the cuff necessary for urine flow interruption is equivalent to bladder pressure. Optional surface EMG electrodes can be applied to the patient’s perineum or abdomen to monitor sphincter activity and abdominal straining, respectively. Following the UroCuff test, a results report is printed which provides pressure-flow data on a modified nomogram.
What are the Advantages of UroCuff Testing?
The advantages of UroCuff testing are numerous, and include:
Non-Invasive
The traditional manner of diagnosing disorders of the lower urinary tract in men is catheterization, which can be embarrassing, uncomfortable, and result in side effects such as injury or infection. Additionally, catheterization may not be appropriate in all patients, particularly those with existing urethral injury. The UroCuff, on the other hand, is completely non-invasive and provides much the same data as traditional pressure flow studies.
Enhanced Patient Compliance
Patients that are prescribed urodynamics testing are more likely to schedule UroCuff testing than invasive pressure flow studies because it is a painless procedure that is less embarrassing than traditional testing.
Repeatable
The UroCuff test can be repeated once every 6 months, giving urologists the ability to better monitor their patient’s symptoms and treatment plan. Patients are less likely to drop out of their treatment plan when progress is easily (and painlessly) monitored.
Lower Cost
UroCuff testing is lower-cost than traditional urodynamic assessment, as it requires less training and is less time consuming. Whereas traditional urodynamics testing requires 30 – 45 minutes to complete, the UroCuff study is finished as soon as the patient’s bladder is empty.
Accurate
Independent studies have proven the accuracy of UroCuff testing in comparison to traditional urodynamic assessment. In one study1 the validity, reliability, and usefulness of the penile cuff was measured in men suffering from lower urinary tract symptoms, such as frequent urination and weak urine stream. For clinical evaluation, 151 men underwent traditional pressure flow studies with a urodynamics catheter in conjunction with UroCuff assessment. The penile cuff could be performed in more than 90% of men with lower urinary tract symptoms, with an accuracy that was statistically similar to what was observed during pressure flow studies.
Can Diagnose Bladder Outlet Obstruction
UroCuff technology has been shown to differentiate disorders such as bladder outlet obstruction in a fully noninvasive manner. At present, 15 – 30%2 of men who are diagnosed with bladder outlet obstruction do not benefit from surgical intervention. This statistic means that careful selection of surgical candidates is necessary, but selection can be difficult. At present, invasive pressure flow studies via catheterization are the gold standard for diagnosing bladder outlet obstruction, but urodynamics via catheterization is not appropriate for all individuals. A definitive diagnosis of bladder outlet obstruction before surgery, however, provides the best surgical outcomes. To verify the utility of UroCuff testing, nineteen men underwent both traditional pressure flow studies and UroCuff assessment for bladder outlet obstruction. In 92% of patients, the UroCuff was able to positively predict bladder outlet obstruction, with sensitivity of 75%. Not surprisingly, 100% of patients preferred this non-invasive method.
When Should UroCuff Testing Be Performed?
UroCuff testing can be performed in many situations. It is most appropriate for healthy men showing symptoms of Benign Prostatic Hyperplasia (BPH). Symptoms of this disorder include uncontrollable urge to urinate, weak urine stream, painful urination, urine leakage, nocturia, and feeling as though the bladder has not been completely voided. Additionally, when bladder outlet obstruction is suspected, UroCuff testing has been shown to be able to provide an accurate diagnosis when compared to traditional pressure flow studies.
Commonly, urologists simply assume that men over 50 with certain lower urinary tract symptoms are suffering from BPH, and prescribe medication without additional testing. UroCuff testing is a simpler and more cost-effect solution than urodynamic assessment, and one for which patients are more likely to be compliant.
For some patients, catheterization can be dangerous. People with existing urethral injury are unable to undergo urodynamic testing, as well as those with an active or recurrent urinary tract infection. However, the information provided by the UroCuff exam is still useful for doctors, making non-invasive UroCuff testing a worthwhile alternative in these situations.
When Should Urodynamics Testing Be Performed?
Despite the advantages of the UroCuff test, invasive pressure flow testing may still be appropriate. For instance, in some cases the UroCuff test may be inconclusive for bladder outlet obstruction, which will require multi-channel urodynamics to be performed. Additionally, the UroCuff does not provide the same wide variety of data as traditional urodynamics testing. One such parameter that cannot be tested for externally is bladder compliance, which is important for the diagnosis of bladder cancer, as well as other lower urinary tract disorders.
There are additional pitfalls that are obvious with noninvasive testing that can make urodynamics a better option. For instance, urodynamics should not be used when acute urinary retention is observed, because the UroCuff is not appropriate for patients with severe lower urinary tract symptoms that prevent them from voiding other than in very small volumes. While traditional urodynamics can also be difficult to perform in this scenario, it is the more appropriate method.
Additionally, when pressure flow studies are required for accurate pressure recordings, urodynamics may still be the more worthwhile test. While UroCuff testing is a useful diagnostic test for problems related to bladder outlet obstruction and BPH, it cannot be ruled out that urethral compression is always equal to pressure during isovolumetric bladder contractions, and that concomitant stricture impeding the flow between bladder and cuff may be a contributing factor. The lack of concomitant intraabdominal pressure limits the ability of Valsalva voiding3 to be measured, which may be necessary in some cases.
For patients with severe lower urinary tract symptoms, traditional pressure flow studies are still preferred. For instance, non-invasive methods are unable to measure the storage phase, which can be important for certain diagnoses. For this reason, the contribution and effect of overactive bladder measurements on bladder outlet obstruction is not well described, and also may be why bladder compliance is unable to be determined. When these variables are necessary, invasive pressure flow studies should always be performed.
How do UroCuff and Urodynamics Fit Together?
When it comes to UroCuff and urodynamics, how do these two techniques fit together? Ultimately, UroCuff is a type of urodynamics test, one that can be performed in conjunction with urodynamics, or separately. UroCuff provides many of the same measurements as would be obtained during invasive pressure flow studies, such as urine flow rate and bladder pressure. This test has shown great utility for diagnosing bladder outlet obstruction, as well. While invasive urodynamics (i.e. catheterization) may still be necessary in some instances, UroCuff can be used for frequent follow up appointments to monitor specific variables during a patient’s care, particularly because there are fewer complications associated with this method, and it is less expensive.
How UroCuff and Urodynamics Complement One Another?
Although UroCuff and invasive urodynamics testing go hand in hand, these two techniques complement one another as well. Since UroCuff provides similar data as urodynamics, it can be used as a non-invasive screening tool. For instance, invasive pressure flow studies are widely avoided by men, due to the pain and discomfort caused by catheterization. Male patients are more likely to consider the non-invasive, external UroCuff due to its pain-free and convenient use. Since the UroCuff provides quantitative data, it can provide additional impetus for patients to undergo invasive testing should there be an abnormality on the UroCuff test, therefore improving patient compliance.
UroCuff is also complementary to urodynamics when physicians strongly assume BPH is to blame for a patient’s symptoms, yet urodynamics is either too costly to perform or the patient is not a good candidate for catheterization. Instead of simply treating the patient for BPH without a definite diagnosis, UroCuff testing can be performed to verify benign prostatic hyperplasia in a cost-effective, complication-free manner.
Finally, the UroCuff complements urodynamics well because it can be performed more frequently – once every six months – at a lower cost to both patient and physician. Since this test is painless, there will be less risk of patients not showing up for testing, which ultimately allows urologists to better monitor their patient’s symptoms and treatment.
The UroCuff is a non-invasive penile cuff that measures urine flow rate while also recording the pressure required to stop the stream of urine. This test can be used in conjunction with, or in place of, traditional pressure flow studies utilized in urodynamic testing. The UroCuff is useful because there is no risk of urinary tract infection or urethral damage, and indeed can be used in patients with either or both disorders. Although the UroCuff has utility for diagnosing BPH and bladder outlet obstruction, it may not be able to replace urodynamics fully. However, the UroCuff is useful when patients refuse urodynamics, as it provides a painless alternative that records quantitative data which can be used to advocate for more extensive testing. The UroCuff is also beneficial because it can be used more frequently than traditional urodynamics, and does not require the same amount of time, money, training, or data interpretation as invasive pressure flow studies. Ultimately, the UroCuff fits together with urodynamics as a complementary tool that has special appeal in many common diagnostic situations.
References
- Harding C, Robson W, Drinnan M, et al. The penile cuff test: A clinically useful non-invasive urodynamic investigation to diagnose men with lower urinary tract symptoms.Indian Journal of Urology : IJU : Journal of the Urological Society of India. 2009;25(1):116-121. doi:10.4103/0970-1591.45549.
- Matulewicz RS, Hairston JC. The UroCuff test: a non-invasive alternative to pressure flow studies in adult males with lower urinary tract symptoms secondary to bladder outlet obstruction. Can J Urol. 2015;22(4):7896-901.
- Matulewicz RS, Hairston JC. The UroCuff test: a non-invasive alternative to pressure flow studies in adult males with lower urinary tract symptoms secondary to bladder outlet obstruction. Can J Urol. 2015;22(4):7896-901.



