Disclaimer: I have not used the new system myself and relied upon colleagues who have for reviews. Additional information is from review of Laborie’s marketing materials.
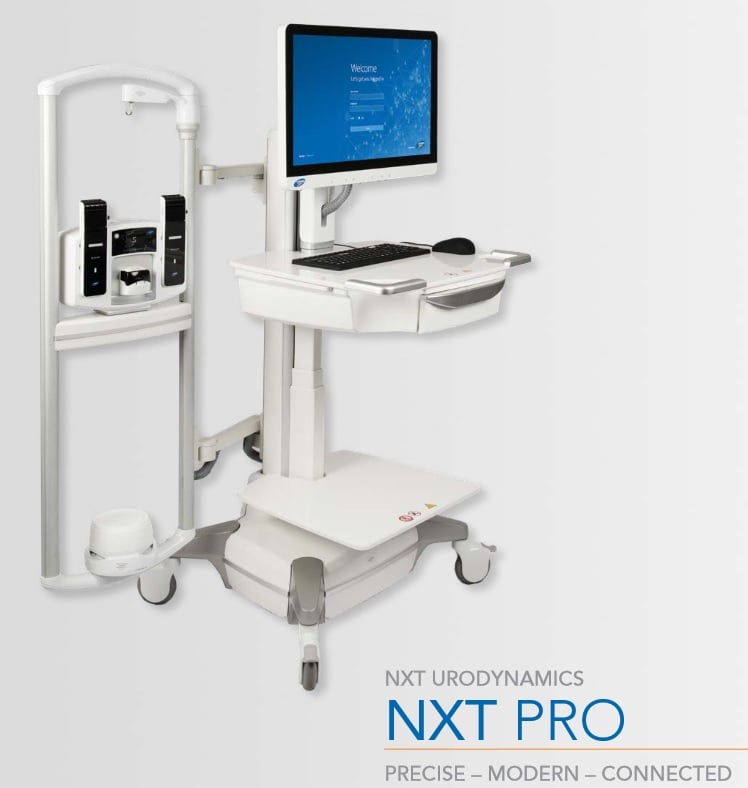
Laborie’s new NXT Pro urodynamics (UDS) system has a variety of features designed to make the user operations simpler and more intuitive. In addition, technological enhancements allow automation of several aspects of the exam and Bluetooth connections to monitoring devices.
Read More
Topics:
Insider,
Urodynamics Testing,
urodynamics,
urodynamics equipment,
urodynamic catheters,
urodynamics service provider
Reimbursement is always a hot topic in urologic care, especially with regards to specific procedures. While individual payors may vary with regards to what they pay for specific evaluation and management (E&M) and procedures (CPT codes), almost all reimbursement is ultimately driven by what rates Medicare will pay and/or how many Relative Value Units (RVU’s) Medicare will assign to a specific E&M or CPT code. This post will review reimbursement trends for urodynamics in 2020 (UDS).
Read More
Topics:
Reimbursments,
urodynamics,
finance,
Reimbursement Trends,
urodynamics billing,
urodynamics profitability
Urodynamics (UDS) is a relatively safe office procedure; however, as with any invasive procedure or test, there are risks associated with performing UDS. A few simple steps can help avoid complications in the majority of patients. Most of the complications associated with UDS are related to urinary tract infections (UTI) and the majority of this blog will focus on that. Additional complications include pain, patient anxiety and injury from catheter placement.
UTI is the most common serious complication of UDS testing, though the frequency of this is difficult to quantify.1 There are excellent guidelines on this from the University of Michigan1 and the American Urologic Association (AUA) also offers guidance for the prevention of UTI’s associated with UDS.2
Read More
Topics:
Urodynamics Testing,
urodynamics service provider,
Medical Practice Operations
Recently, a large-scale study of men referred to urologists in England for difficulty urinating has published results (Lewis Eur Urol 2019). This trial, called UPSTREAM, recruited over 800 men for two dozen locations across England. In addition to the usual history, physical and baseline evaluation for the voiding issues, some men were randomized to undergoing a urodynamics test (UDS) and the authors have recently reported some of their data.
Read More
Topics:
Urodynamics Testing,
male urodynamics,
Male Diagnostics
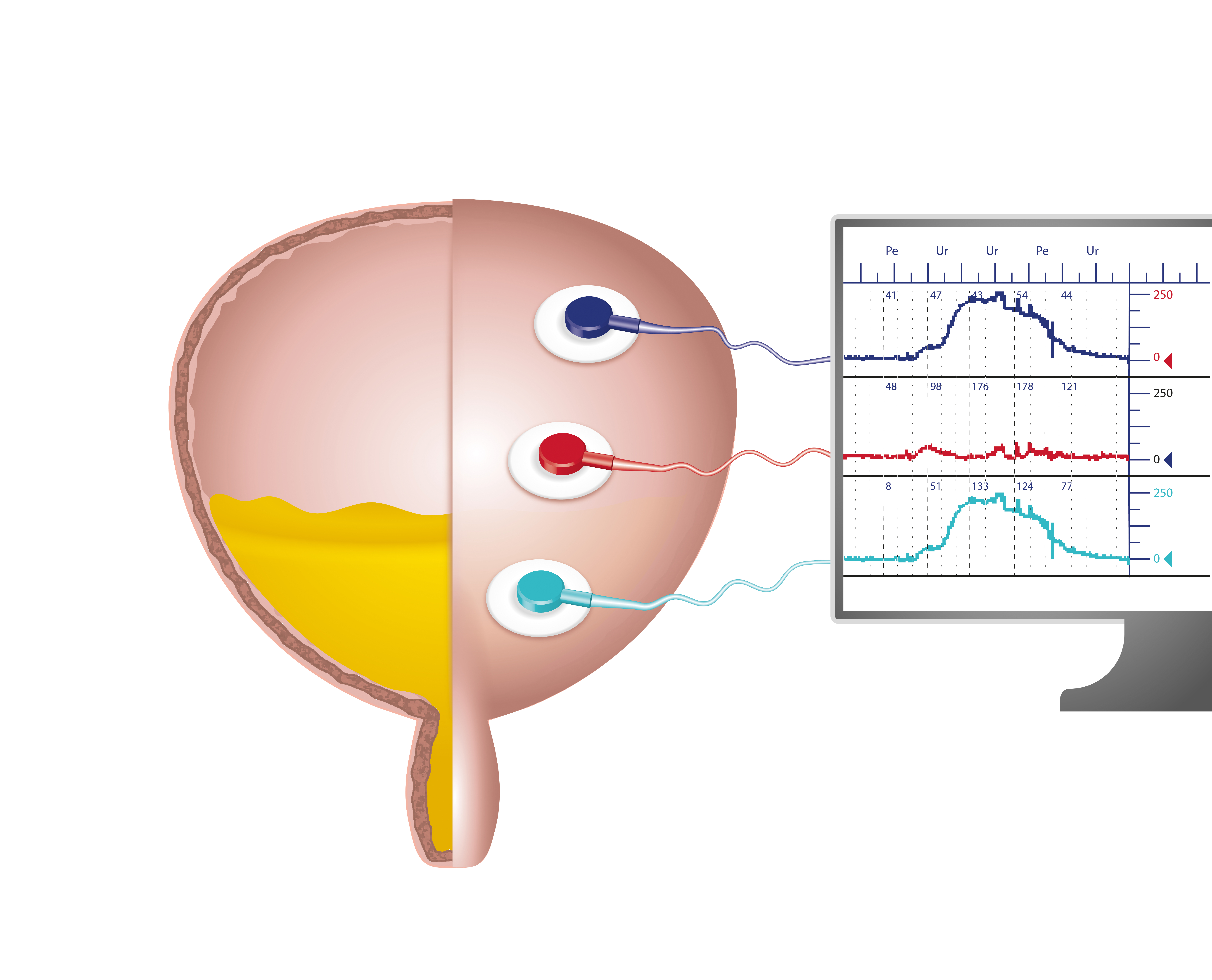
During a urodynamics study (UDS), there are a variety of pieces of data coming in to the urologist and technician performing the study. Information will be obtained that is both subjective and objective in nature and the question is, who do you believe? Do you believe yourself and the objective data you are reviewing? Or, do you believe what the patient is telling you during the study? This blog post will explore this in detail.
Read More
Topics:
Urodynamics Testing,
urodynamics training,
urodynamics interpretation
Urodynamics (UDS) testing is usually performed in conjunction with a slew of other urologic tests and functions in concert with other diagnostics. This blog post will explore other common tests used in patients who will be having UDS testing and explains the indications and data that come from those other assessments.
All patients who have UDS will undergo a comprehensive history, physical and laboratory testing. The history will focus on the specific urologic complaints the patient has, but also bowel issues, neurologic disorders and whatever medications the patient is on as well. Surgical history, especially related to urinary tract and anti-incontinence surgery is critical as is diet information. Lab testing will include a urinalysis to search for blood or infection, urine culture if infection is suspected, and many patients will have serum lab testing to assess kidney function.
Read More
Topics:
Urodynamics Testing,
outsourcing diagnostics,
urodynamics service provider,
Uroflowmetry,
Urology Practice Trends,
Post-Operative Urodynamics
Since urodynamics (UDS) is a relatively time consuming test, physicians who perform and interpret UDS are reliant on ancillary medical staff to perform much of the UDS study. This role is often performed by a mid-level provider, such as a nurse practitioner (NP), physician’s assistant (PA), registered nurse (RN) and even by a medical assistant or other trained technician (MA). The degree of medical knowledge needed to successfully perform a UDS test does not need to be extensive, hence providers do not need a medical or advanced degree to perform UDS; however, they do need to be proficient in setting the patient up for the test, know the key steps, know how to manage basic artifacts and when to engage the physician during a test.
Read More
Topics:
Urodynamics Testing,
urodynamics equipment,
urodynamics training
UDS is a critical procedure in the practice of urology and the management of voiding dysfunction in men and women. All urologists receive exposure to UDS testing during residency training. In the United States, residents are required to perform and interpret 10 UDS studies in order to graduate from residency. In addition, some residents choose to undertake fellowship training in Female Pelvic Medicine and Reconstructive Surgery (FPMRS), where substantial exposure to UDS is had. UDS testing certainly is utilized in significantly more patients and a part of care for many other patients encounter during training; however, as with many other skills, there will be a wide range of exposure during training and quality will certainly vary between programs.
Read More
Topics:
urodynamics,
urodynamics training,
clinical operations,
urodynamics service provider,
Medical Practice Operations
As with many of the practical aspects of urodynamics (UDS) testing, the rate at which the bladder is filled during the cystometric portion of the exam influences the test results. Generally speaking, filling during UDS can be at rates below physiologic levels, at physiologic levels or at supra-physiologic levels. There are distinct pros and cons to filling at either physiologic rates or rates above that, while filling at a rate below the natural rate of bladder filling is both inefficient and unnatural.
Read More
Topics:
Urodynamics Testing,
urodynamics,
urodynamics training
As with many aspects of medical practice, a solid training foundation is critical to best practices and the safe delivery of care. When it comes to performing urodynamics (UDS), as with many other procedures, the question of what level of training is requisite to perform UDS appropriately is a reasonable one. And the natural extension of this is whether or not a specific certification process is warranted to perform UDS.
Read More
Topics:
Urodynamics Testing,
urodynamics,
urology,
UroGynecology