When it comes to conditions of the lower urinary tract, there are key differences to consider in order to determine which form of testing is the most appropriate. While there are striking similarities between methods that can potentially create confusion upon first glance, a practitioner knows which test is most appropriate for the corresponding symptoms.
One area that has the potential to create this confusion is determining the difference between the need for the broader Urodynamics testing panel or the Cystometrogram. While these two procedures involve many of the same elements, they are in fact different.
This post will provide a detailed comparison of the two methods and describe how they are similar, but also different. First, a brief explanation of the two methods before we compare:
Read More
Topics:
Urodynamics Testing,
BHN,
outsourcing diagnostics,
urodynamics,
incontinence,
urodynamics service provider,
male urodynamics,
stress incontinence,
Uroflow,
Uroflowmetry,
UroGynecology,
Cystometrogram
An aging US population brings unique challenges to urologists and the urology workforce in general. As the average age of the population increases, this means that the frequency of urologic diseases and need for urology-related treatments also increases, and it is having an effect on the industry in general as demand increases. These demographic changes in the United States are in turn changing the demands on the urology workforce, creating a need by professionals to have the latest data, research, education, and advocacy for a changing industry.
With the findings published in the American Urology Association’s 2020 census, along with comparisons with their previous publications, we can form a clear picture of what the urology workforce and industry has been through in the past, what it is currently dealing with as of the 2020 publication, and we can also infer educated predictions about the future to anticipate what urologists and urology professionals will need to prepare for in order to meet the growing demand for urology care.
Here is a summary of some of the key findings of the AUA’s 2020 census:
Read More
Topics:
Urodynamics Testing,
urodynamics,
urodynamics staffing,
incontinence,
clinical operations,
urology,
urodynamics service provider,
Medical Practice Operations,
Uroflowmetry,
UroGynecology
Urinary incontinence can provide health care professionals with a challenge that may seem like it requires surgery when there are in fact a range of nonsurgical and even non-pharmacological options that can be employed first. To experienced urologists, this will be apparent, however other healthcare professionals who do not have a full working knowledge of urodynamic testing along with urinary incontinence treatment options may choose surgery or medication when there are many steps that can be taken and explored before resorting to more invasive options.
An Overview of Urinary Incontinence
Read More
Topics:
Urodynamics Testing,
urodynamics,
urinariy incontinence,
incontinence,
clinical operations,
urology,
urodynamics service provider,
male urodynamics,
UroGynecology
2020 and 2021 have shown that urodynamics continues to grow and find unique and novel applications for diagnosing health issues relating to the bladder, urethra, and more. Here we have outlined 4 of the most interesting studies of the past year in the world of urodynamics:
Read More
Topics:
urodynamics,
urodynamics training,
urodynamics staffing,
incontinence,
urodynamics interpretation,
urodynamics service provider,
Urology Practice Trends,
UroGynecology
One of the most vexing clinical situations happens to be one of the best uses of urodynamics (UDS): ongoing symptoms after female incontinence surgery. These cases are challenging and patients are often not happy to have ongoing symptoms, new symptoms or worsening symptoms; however, appropriately utilized and interpreted, UDS can be key to helping these patients.
Read More
Topics:
Urodynamics Testing,
urodynamics,
incontinence,
Post-Operative Urodynamics
Bladder cancer is a relatively rare phenomenon in the United States – affecting fewer than 200,000 Americans annually – but can be serious when left untreated. Here, incontinence will be discussed relative to bladder cancer, which is a side effect of both the cancer itself and the treatment.
Read More
Topics:
incontinence,
Bladder Cancer
Incontinence is an uncomfortable subject that affects millions of men and women worldwide. Traditionally, an incontinence sufferer would visit his or her primary physician and then be referred to a urologist, depending on symptom severity. Recently, a number of OB-GYN practices have begun offering incontinence care. Here, whether OB-GYN practices should provide care for incontinent patients will be discussed.
Read More
Topics:
urodynamics,
incontinence,
ObGyn Practices
Urodynamic testing is the gold standard for incontinence assessment; however, this method is not without
drawbacks. For instance, data interpretation is reliant on a number of factors, including the clinician’s training, proper use of the equipment, and reproduction of the patient’s symptoms during testing.
Read More
Topics:
urodynamics,
incontinence
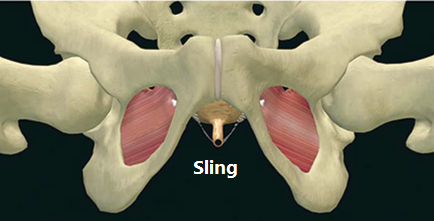
Sling Procedures are not a new phenomenon; after all, the original Sling Procedure was performed in 1907 by Von Giordano utilizing a gracilis muscle graft around the urethra. Since then, a number of improvements have been made to the Sling Procedure, particularly in the past 15 years. Sling Procedures over the last decade will be summarized here.
Read More
Topics:
urinariy incontinence,
incontinence
The consequence of incontinence extends far beyond embarrassment. Around 13 million people in the U.S. have been diagnosed with incontinence, according to the Agency for Healthcare Research and Quality. While older age increases the risk of this condition, there are a wide range of factors that can cause this problem in younger persons. Meanwhile, women are much more likely than men to experience incontinence, per the Centers for Disease Control.
Read More
Topics:
urodynamics,
urinariy incontinence,
incontinence